Authored by David Wagner (BS Brain & Cognitive Sciences) & Edited by Gaurav Dubey (MS Biotechnology)
High-Quality, Evidence-Based Scientific Content Brought to you by Karmik, LLC
This blog was initially published here at EvolveIndy.com. To read the full post and learn more about the “Spheres of Awareness” and how they challenge the status quo of addiction research.
Drug addiction is a pervasive public health issue throughout modern western society, afflicting individuals across all socioeconomic stratifications, races, genders, and ethnic backgrounds. Each year, significant medical and economic resources are deployed to treat drug and alcohol addiction, and yet, despite the politico-medical effort to stalwart the “disease” of addiction, it remains one of the most pressing social issues of our time. Currently, modern science and addiction medicine have failed to produce an effective, universal answer for resolving drug addiction, instead relying on big pharma to reverse engineer a solution to a problem they have largely created, or rehabilitation programs based on 12-step facilitation (TSF) that have questionable clinical efficacy and effectiveness.1, 2
Indeed, the current (and past) focus of drug addiction treatment (and for many, subsequent involvement in the criminal justice system) seems to reinforce a contraction of consciousness and brain activity, continued dependence on mind-altering substances, and a triggering of core trauma through punitive care models. Understanding and applying information about states of consciousness, rooted in transpersonal psychology and modern cognitive science, could provide a platform for a new lens to view addictive behavior and, more importantly, for how to develop effective strategies to transmute those brain states into integrated functioning.

The Development of the Modern Addiction Treatment (Management) Model
Modern addiction treatment has progressed immensely from its dark roots. William White’s 1998 book, Slaying the Dragon: The History of Addiction and Treatment in America, provides an archival presentation of the formation of today’s addiction treatment model. The book follows the placing of alcoholics and addicts on inebriate farms in the early 1900s, the utilization of narcotic drugs for dependency maintenance in the 1920s, psychosurgery and electroshock therapies in the 1940s, and the formation of specialized TSF rehabilitation centers in the mid-century— the model of treatment that has remained largely unchanged since. Furthermore, the combination of TSF-based addiction treatment and the criminal justice system in the early 90s, with the creation of drug treatment courts and court-mandated substance abuse treatment, provided the combination of law enforcement and the promise of medicine to create a new platform for managing addiction. In the last decade, the reemergence of the wide scale use of narcotic and psychotropic medications to manage dependency and treat underlying psychological issues has become the standard of care. The combination of medication therapies and TSF-based rehabilitation is the current gold-standard in addiction care and management, and by some accounts contributes to a decreased overdose rate, decreased risk of relapse, and a reduction in infectious diseases like HIV.3
On The Surface, It Would Appear We’ve Optimized a More Efficacious Treatment for Managing Addiction
On face value, it would appear that we have optimized a system for managing addiction as a chronic illness and compared to previous attempts in history to manage addicts, it seems as though we have moved to a better standard of care of addiction management. The ideal goal of successfully treating and resolving addiction, however, seems to have been lost in the current model of addiction management. In the context of addiction management, we have shifted the entire idea from resolving the roots of addiction and addictive behavior to psychopharmaceutical and behavioral management (generally through negative reward reinforcement at least in current models of treatment). It may well be time to update the management-based approach to addiction to incorporate ideas and practices that could help the addict change the brain state employed addiction and transform their baseline level of consciousness away from the contracted state of consciousness that addiction itself facilitates and the dissociated state of consciousness that the current management-based system may serve to maintain.
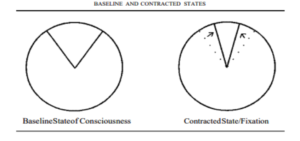
Addiction as a Contracted State of Consciousness: The Spherical Field of Awareness Thought-Model
Ralph Metzer proposed a thought-model of consciousness as a “spherical field of awareness that surrounds us and moves with us everywhere we go”.4 For simplification purposes, we will work with one 2-D slice of this sphere of consciousness. This horizontal plane section of the spherical field gives us a 360° circle of “potential awareness,” or a potential focus of attention. We will assume that in our baseline state of consciousness we utilize only 45° of the available 360° consciousness field.

In Active Addiction, Our Attention Becomes Extremely Narrow
In active addiction, our attention becomes extremely narrow; our focus on a singular purpose (getting and using our drug of choice) becomes hyper-vigilant, and our brain activity becomes more organized and synchronous (resulting in a net increase in rigidity or decrease in adaptability). We effectively decrease our field of potential awareness down to 30°, or 15°, or even just 1° of the total possible experience of consciousness. The external object of desire, the craved sensation, the bottle, pipe, etc., becomes the slice of potential awareness we occupy; the remaining field of potential awareness is completely excluded from our narrow band of reality.
Contracted States of Consciousness Can Be Useful In Accomplishing Tasks, But Damaging As a Permanent Brain State
This contraction of consciousness is a very useful state for accomplishing tasks that require extreme focus and attention to detail in the short-term, but in the addicted individual it becomes a pathological state of narrow fixation, repetition, and eventually ritualistic behavior. The brain adapts to this state of hyper-focus and the subsequent positive feedback from the reduction in anxiety (fear) that the drug provides. We essentially train our brain to work against its own innate programming to expand.
Consciousness in Contracted Brain States
There is a central tenant in modern neuroscience that conveys the basic idea of how thoughts become behaviors hard-wired in the brain; this is the idea of “neurons that fire together, wire together”.5 When groups of neurons repeatedly fire together they form what is called a neural network. Neural networks are thought to represent hard-wired “circuits” of our conscious experience, behavior and memories in our brain’s architecture. Their activation creates a signature pattern of brain activity. Additionally, there are patterns of brain activity that are always occurring, whether we are in our waking state or in states of altered consciousness (such as deep sleep, dreaming, etc.). These patterns of on-going activity are thought to represent a neural correlate of consciousness (NCC) and is postulated to be the framework that builds our conscious experience.6 These patterns of activity are modified from sensory inputs to improve our understanding of the world around us, and can be built from a nearly infinite number of neuronal connections, representing a nearly infinite number of brain states or slices of consciousness. In a contracted brain state, the number of possible patterns of activity is reduced to a much smaller subset. These certain patterns of activity become reinforced by coordinated firing of neurons driven by a narrow focal point of external stimuli. If the reward (reduction of fear being a highly-prized reward in our brain) of obtaining or ingesting that stimuli is large enough, the brain adapts to these patterns of activity and essentially begins to recode itself with access to a much more limited number of activity states.
Epileptic Seizures As an Example of Contracted Brain States
The most grievous example of a contracted brain state is what happens during an epileptic seizure; instead of an alteration of synchronous and differentiated firing of high informational complexity , the patterns of brain activity become rigidly synchronous and simple. Consciousness becomes altered and narrowed to a very limited band of functioning in the person having an epileptic seizure. Patterns of brain activity are selected from a very simple, limited number of possible brain states and repeated until the seizure state is arrested.
The Process of Drug Addiction Follows a Similar Pathology to Epileptic Seizures
The process of drug addiction and the subsequent contracting of consciousness follows a similar pathology as the epileptic seizure: rigidity in brain activity, narrowing of the selection of possible brain activity states, simplification and reduction of neural entropy, and the reinforcement and adaptation to a small subset of brain activity patterns. The brain ceases to function in its innate, immense processing and integrative abilities, given the focus on an external object, and the sole purpose of its function becomes the maintenance of a contracted slice of awareness. Treatments for drug addiction that reinforce rigidity in brain activity (black and white thinking) and induce fear and anxiety (punitive consequence of relapse, either through the criminal justice system or from social isolation from self-help groups) should all be regarded as highly dubious, based on this conceptualization of addiction as a form of contracted consciousness/brain states. The therapy intended to treat addiction may well reinforce its hold on us more deeply in these models of treatment.
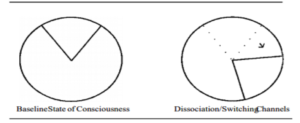
Dissociation Changes Consciousness and Brain states, But Doesn’t Expand Them
One of the common issues in early drug addiction recovery is a phenomenon known as pseudo-transcendence. The idea here is that we shift our narrow band of focus within the 360° potential of awareness to another restricted area within the circle. If we were to imagine our drug addiction experience as watching the same television program over and over, we simply switch the channel to a new program and repeat the cycle of repetitively viewing a new program. Instead of expanding the repertoire of brain states and patterns of brain activation, we are simply replacing a small set of highly predictable activations with different small set of highly predictable activations. Switching addictions from drugs to sex, gambling, working, people-pleasing, and all manners of dissociative behavior are not uncommon in early recovery processes. The addicted brain has been well trained to work in narrowing bands of focus to achieve the resolution of painful internal trauma, and adapts easily to these familiar patterns with a new, novel external stimulus . And again, the more these patterns of brain activity occur together, the more deeply they’re ingrained in our behavior and breadth of conscious awareness.

Channel-Switching Therapies: Effective Reprieve or New Addiction Unto Itself?
Channel-switching therapies can be effective as a reprieve from the previous behavioral patterns, leading to a reduction in anxiety and the compulsive behaviors utilized to self-medicate. They can also quickly become a new source of fixated and compulsive behavior, as the idea here isn’t the resolution of painful internal states, but the management of anxiety caused by these states through change in attention and focus. The psychoactive, mood-altering medications (SSRIs like Prozac, gabapentin, mood stabilizers like Abilify and anxiolytics like Klonopin), often dispensed to addicts in early recovery, are a prime example of channel-switching, as they alter consciousness without any expansion of consciousness. Some reduce brain activation or interfere with new neuron development, and provide quick (or moderately quick) management of distressing symptoms; none of these medications help the addict confront the underlying issues driving their contracted state of awareness, and potentially separate them further from discovery due to their dissociative effect.
The Problem with Opioid MAT (Medication Assisted Treatment) Therapy
Long-term opiate maintenance therapy is the epitome of dissociative therapies. Dr. Stuart Gitlow, past president of the American Society of Addiction Medicine, says, “The drug that we’re replacing is a dangerous one that will kill you, and we’re replacing it with a drug that allows you to go back to work and have money in your pocket and allow you to live normally again”.7 In Wisconsin’s 2016 Calendar Year Report on Opioid Treatment Programs, however, 6669 of 9568 patients in opioid treatment programs (69%) were funded by Medicaid, which implies that the majority of the population receiving these treatments are either unemployed, under-employed, or disabled, given that this is a key qualifier for these benefits.8 So yes, substitution MATs may be preventing or reducing overdose deaths, but probably not fulfilling the genuine return to productivity as Dr. Gitlow claims. Additional issues with MATs, and why they should be viewed as a dissociative therapy at best, are: the further impairment of neuronal circuit plasticity, continued integration of maladaptive brain states that develop from opiate misuse, and, in general, keeping the addicted person subservient to a process of ritualistic drug use as a rewarding behavior.
A Note About Mindfulness and Other “New Age” Psychotherapies
Transcendental meditative practices and certain “new age” psychotherapeutic techniques also fall into this realm of channel-switching consciousness, as they function to distract attention from the internal source of the problem through fixation on a repeated mantra or affirmation. 12-step programs can also dip into the realm of a channel-switching therapy, as when priority is given to the social interaction the group provides, or relief of internal anxiety through mere attendance replaces actual application of the spiritual principles divulged in 12-step literature as a program of recovery. As should be clear, pseudo-transcendence or channel-switching is clearly a shift in consciousness from one plane of maladaptation to another.
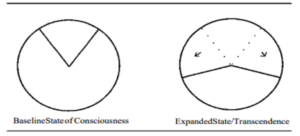
This blog was initially published here at EvolveIndy.com. To read the full post and learn more about the “Spheres of Awareness” and how they challenge the status quo of addiction research.
Works Cited:
- Kownacki, R. & Shadish, W. Does Alcoholics Anonymous work? The results from a meta-analysis of controlled experiments. Subst Use Misuse. 34 (14), 1897-1916 (1999)
- Ferri, M., Amato, L., & Davoli, M. Alcoholic Anonymous and other 12 step programmes for dependence. https://doi.org/10.1002/14651858.CD005032.pub2
- Schwartz, R. et al. Opioid Agonist Treatments and Heroin Overdose Deaths in Baltimore, MD 1995-2009. AM J Public Health. 103 (5), 917-922 (2013)
- Metzner, R. Addiction and transcendence as altered states of consciousness. J Transp Psych. 26, 1-17 (1994)
- Lowell, S. & Singer W. Selection of intrinsic horizontal connections in the visual cortex by correlated neuronal activity. Science. 255, 209-212 (1992)
- Ward, L. The thalmic dynamic core theory of conscious experience. Consciousness and Cognition. 20, 464-486 (2011)
- https://www.statnews.com/2017/05/15/medication-assisted-treatment-what-we-know
- https://www.dhs.wisconsin.gov/publications/p02115-16.pdf
- Goyal, M et al. Meditation programs for psychological stress and well-being: a systematic review and meta-analysis. JAMA Intern Med. 174 (3), 357-368 (2014)
- Tang, Y., Tang, R., & Posner, M. Mindfulness meditation improves emotional regulation and reduces drug abuse. Drug and Alcohol Dependence. 163 (1), S13-S18 (2016)

Recent Comments